
Recent news

Laughing gas
2024.04.23
Blood test can detect laughing gas and help the police fight dangerous tendency

Air pollution
2024.04.22
High air pollution in Denmark may impact children's academic performance

Atoms
2024.04.22
Superradiant atoms could push the boundaries of how precisely time can be measured

Family life
2024.04.20
New research: Danish children encounter four typical family learning environments

CLIMATE
2024.04.18
Increased CO2 emissions from world’s tundra surprise researchers

Mental health
2024.04.17
Fluctuating coffee prices put mental pressure on Vietnamese farmers

Quantum Data
2024.04.15
Internet can achieve quantum speed with light saved as sound
species
2024.04.12
Iconic savanna mammals face genetic problems due to fences and roads

Sonning Prize
2024.04.11
After stroke: Marina Abramović to receive the Sonning Prize

poverty
2024.04.11
Economist: Tens of billions of dollars in forest products are being overlooked
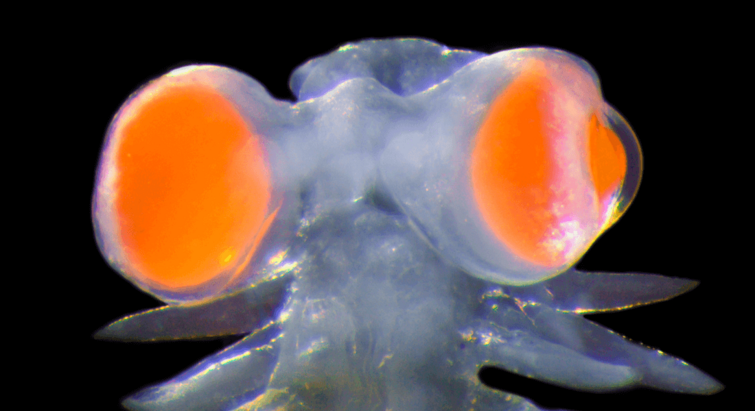
Marine Biology
2024.04.09
Mediterranean marine worm has developed eyes “as big as millstones"

Diversified farming
2024.04.05

